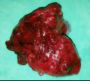
Spontaneous Hemoperitoneum Due To Necrotic Omental Tumour-A Case Report
Abstract
Hemoperitoneum due to bleeding from
intra-abdominal tumours is relatively
rare. We report an unusual case of acute
abdomen with hemoperitoneum due to
bleeding from omentum mimicking a tumour
bleed. A 25 year-old-male presented
to us with complaints of abdominal
pain and distention. Computed tomography
revealed a 12 x10 cm heterogeneous
mass along the greater curvature
of stomach with significant hemoperitoneum.
An emergency laparotomy was
performed. Intra-operatively, 3000 ml of
dark blood, and a hemorrhagic necrotic
mass in the gastrosplenic omentum was
found. Resection of the mass was performed.
Histopathology revealed a hemorrhagic
necrotic mass, with no viable
tissue. Since there was no viable tissue,
the nature of the tumor could not be diagnosed.
Regular follow-up is planned in
view of the uncertain nature of primary
tumour. The differential diagnosis includes
a wide variety of benign and malignant
tumours, trauma, infarction and
vascular causes. Omental tumours
should be included in the differential diagnosis
of spontaneous hemoperitoneum.
The treatment of choice is complete excision
of the tumour in view of the multitude
of causes and possibility of malignancy.
Full Text:
PDFReferences
Ho MP, Chang CJ, Huang CY, Yu
CJ, Tsai KC, Chen HA, et al. Spontaneous
rupture of the short gastric
artery after vomiting. Am J Emerg
Med 2012;30:513 e1-3.
Lucey BC, Varghese JC, Soto JA.
Spontaneous hemoperitoneum:
causes and significance. Curr Probl
Diagn Radiol 2005;34:182-95.
Cawyer JC, Stone CK. Abdominal
apoplexy: a case report and review.
J Emerg Med 2011;40:e49-52.
Fernández-Rey CL. Primary
omental infarction as cause of nonsurgical
acute abdomen: imaging
diagnosis. Rev Esp Enferm Dig
;102:498-9
Peirce C, Martin ST, Hyland JM.
The use of minimally invasive surgery
in the management of idiopathic
omental torsion:
The diagnostic and therapeutic role of
laparoscopy. Int J Surg Case Rep
;2:125-7.
Pérez-Navarro JV, Flores-Cardoza A,
Anaya-Prado R, González-Izquierdo Jde
J, Ramírez-BarbaEJ. Angiofibrolipoma
of the greater omentum: case report and
literature review. Cir Cir 2009;77:229-
Chien JC, Lao WT, Chen CL, Chan
WP. Follicular dendritic cell sarcoma of
the omentum: multidetector computed
tomography findings. Korean J Radiol
;14:213-7.
Schwartz RW, Reames M, McGrath
PC, Letton RW, Appleby G, Kenady DE.
Primary solid neoplasms of the greater
omentum. Surgery1991;109:543-9.
Miyano G, Hayashi T, Arakawa A,
Goto S, Lane GJ, Okazaki T, Yamataka
A. Giant omental lipoblastoma and
CD56 expression. Afr J Paediatr Surg
;10:32-4.
Harano K, Ando M, Sasajima Y,
Yunokawa M, Yonemori K, Shimizu C,
Tamura K, Katsumata N, Tsuda H, Fujiwara
Y. Primary yolk sac tumor of the
omentum: a case report and literature
review. Case Rep Oncol 2012;5:671-5.
Zong L, Chen P, Wang GY, Zhu QS.
Giant solitary fibrous tumor arising from
greater omentum. World J Gastroenterol
;18:6515-20.
Ben Achour J, Bouasker I, Bedoui R,
Daghar K, Ayari H, Guesmi F, et al.
Myofibroblastic tumor of the great omentum.
Tunis Med 2008;86:932-5.
Chen SS, Chen CP, Chien SC,
Hsu CY. Spontaneous rupture of
omental teratoma mimicking a ruptured
ovarian teratoma. Taiwan J
Obstet Gynecol 2008;47:229-32.
Fernandes R, Dhillon B, Andrews
B. Haemoperitoneum secondary
to rupture of an omental artery
aneurysm. BMJ Case Rep.
0 0 9 ; 2 0 0 9 . d o i : p i i :
bcr06.2009.2047. 10.1136/
bcr.06.2009.2047.
Umiker WO, Iverson L Postinflammatory
tumors of the lung; report
of four cases simulating xanthoma,
fibroma, or plasma cell tumor
J Thorac Surg1954;28:55–63
Gleason BC, Hornick JL Inflammatory
myofibroblastic tumours:
where are we now? J Clin
Pathol2008;61:428–437
Sodhi KS, Virmani V, Bal A, Saxena
AK, Samujh R, Khandelwa N.
Inflammatory pseudotumor of the
omentum. Indian J Pediatr. 2010
Jun;77(6):687-8.
Singhal M, Ramanathan S, Das
A, Gurpreet Singh, Baggad R,
Khandelwal N. Omental inflammatory
myofibroblastic tumour mimicking
peritoneal carcinomatosis. Cancer
Imaging 2011;11:19-22
Narla LD, Newman B, Spottswood
SS, Narla S, Kolli R Inflammatory
pseudotumor RadioGraphics
;23:719–729
Xue D, Chen H, Chen Y. Giant
extragastrointestinal stromal tumor
in the transverse mesocolon concomitant
with gastric
cancer in an elderly patient: Case
report. Oncol Lett 2013;5:627-30.
Fletcher CD, Berman JJ, Corless
C, Gorstein F, Lasota J, Longley BJ,
et al. Diagnosis of gastrointestinal
stromal tumors: a consensus approach.
Hum Pathol 2002;33:459–
Reith JD, Goldblum JR, Lyles
RH, Weiss SW. Extragastrointestinal
(soft tissue) stromal tumors: an
analysis of 48 cases with emphasis
on histologic predictors of outcome.
Mod Pathol 2000;13:577-85.
Barros A, Linhares E, Valadão
M, Gonçalves R, Vilhena B, Gil C,
et al. Extragastrointestinal stromal
tumors (EGIST): a series of case
reports. Hepatogastroenterology
;58:865-8.
Llenas-García J, Guerra-Vales
JM, Moreno A, Ibarrola C, Castelbon
FJ, Fernández-Ruiz M, et al.
Primary extragastrointestinal stromal
tumors in the omentum and
mesentery: a clinicopathological
and immunohistochemical study.
H e p a t o g a s t r o e n t e r o l o g y
;55:1002-5.
Refbacks
- There are currently no refbacks.

This work is licensed under a Creative Commons Attribution-NoDerivatives 4.0 International License.
An Initiative of The Tamil Nadu Dr MGR Medical University
 University Journal of Surgery and Surgical Specialities
University Journal of Surgery and Surgical Specialities